Do you turn to alcohol to cope with feelings of depression? Maybe you drink to forget about a painful breakup or to relieve the stress of your job. While alcohol may provide temporary relief, it can lead to a dangerous cycle of using alcohol to manage negative emotions. Research shows that people struggling with alcohol use disorder (AUD) are three times more likely to experience major depression. This connection isn’t coincidental. Alcohol and depression often feed into each other, creating a destructive cycle that can be hard to break. Understanding depression, its various forms, and how it interacts with alcohol use is the first step toward breaking this cycle.
Types of Depression:
Like many mental disorders, various types of depression have different causes. Here are the most common types of depression and how they can appear:
- Situational Depression: This type of depression does not count as disordered depression or sadness. Situational depression refers to the melancholic mood that all people get into after a distressing event. The depressed mood you feel in situational depression is in direct response to an event and typically subsides over time. For example, it is typical for someone to feel depressed after the death of a family member or a divorce. Through the passage of time and/or support from loved ones, situational depression becomes manageable and eventually passes.
- Major Depressive Disorder (MDD): People who suffer from major depressive disorder feel persistent depressive moods the majority of the time. Common symptoms are the loss of interest in what once was exciting, feeling sluggish and unmotivated, and trouble making decisions. People with MDD may also experience physical symptoms like weight loss/gain, lack of energy, and slowed body movements.
- Seasonal Affective Disorder (SAD): People with SAD feel the same symptoms of major depressive disorder, except only within particular seasons. For most people, symptoms of SAD flare up in the winter months. This is explainable by the wealth of research findings, a strong association between shorter days/lack of sunlight and depression.
- Persistent Depressive Disorder: Previously called “dysthymia”, this disorder is classified as experiencing depression symptoms for two consecutive years. Although people with this disorder may have periods of major depression, their typical symptoms are usually less severe, although long-lasting.
- Postpartum Depression: Postpartum depression is the depression a person may experience after childbirth. This is not to be confused with “baby blues”, which have similar symptoms to postpartum depression, but only last for about a week after birth. Postpartum depression can start during pregnancy and last many months after giving birth. Symptoms like severe mood swings, feelings of hopelessness, difficulty bonding with the baby, and severe anxiety make this disorder extremely difficult to deal with while caring for a newborn.
Beyond these few, there are many other forms that depression can take and similar disorders that may look like depression on the surface. If you think you may be experiencing depression or a related condition, talk to your doctor and reach out to trusted people for help.
Depression Symptoms
Symptoms may vary from person to person, depending on each individual’s circumstances. Not all symptoms may be present, and other symptoms not appearing on this list may be related to depression.
Some common symptoms associated with depression and related disorders are:
- Persistent feelings of sadness, hopelessness, negativity, or emptiness
- Loss of interest or excitement in hobbies or other activities previously enjoyed
- Thoughts of harming oneself
- Trouble concentrating, recalling information, sleeping, and/or awakening
- Change in appetite
- Reduced energy
- Headaches, body aches, or other discomforts with no clear physical cause
- Emotional outbursts, which may include shouting, screaming, or crying
- Feelings of insecurity, guilt, or shame
If you or a loved one has been experiencing one or more of these for a prolonged period (often at least two weeks) and/or they’re negatively impacting you at home, work, or school, talk to your doctor about the possibility of depression. Certain symptoms may be more severe than others, and a few carry a higher risk, especially relating to self-harm. Professional advice, particularly mental health care, should be sought immediately when thoughts of harm are involved.
Risk Factors and Causes of Depression
Depression can affect anyone at any time, regardless of age, race, gender, income, or other demographic differences. There are, however, genetic, environmental, physiological, and other factors that increase an individual’s risk of developing depression. The factors that tend to most impact someone’s risk include:
- Family history
- Physical illness or injury
- Medications
- Trauma
- Major life changes
Although there are clear risk factors for developing depression, no one knows exactly what causes it. One thing that psychologists do know is that biological differences in someone’s brain chemistry can play a large role in the development of depression and other mood disorders. Specifically, recent research indicates that changes in certain chemicals or neurotransmitters in the brain may contribute to someone’s risk of depression. Hormone changes in the body can also contribute to depression, as is often the case with postpartum depression. However, not everyone who has brain differences or hormonal changes develops depression, so these factors can’t be proven causes of the disorder.
Researchers also consider co-occurring disorders by studying the causes and risks of mental health conditions. Depression often occurs alongside another mental health disorder or medical problem. Those with existing mental health conditions like ADHD, PTSD, anxiety, and others are at a higher risk of developing depression, as are those with illnesses like cancer, multiple sclerosis, Parkinson’s, and more. Those with a dual diagnosis of two existing disorders need to address both issues in treatment to find long-term relief.
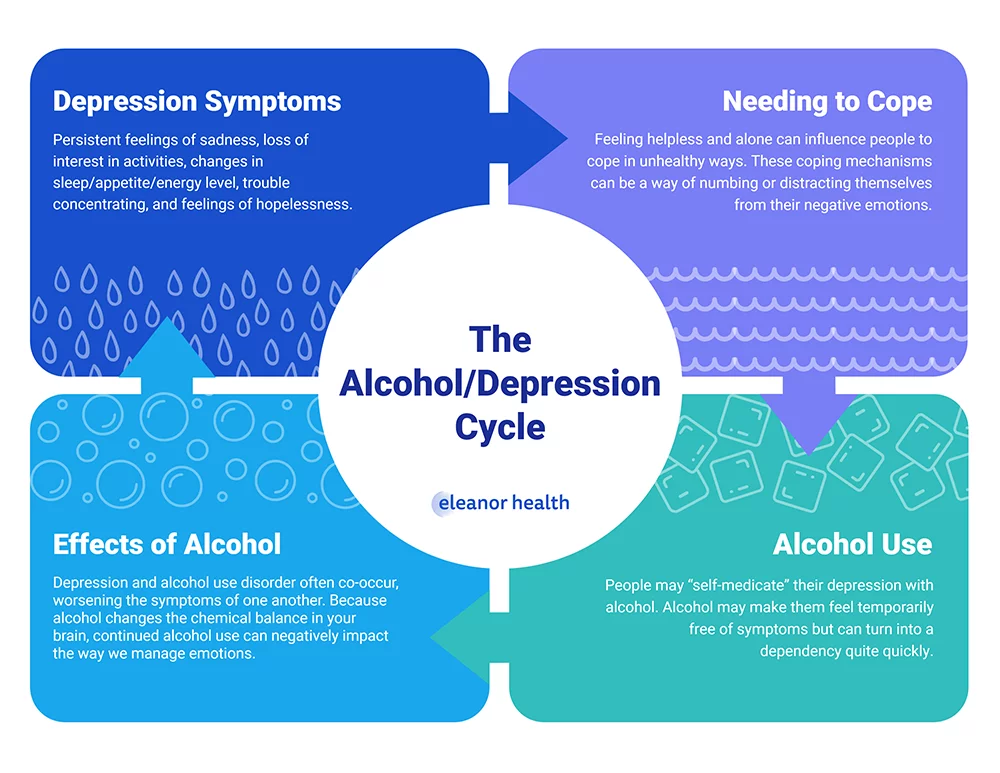

The Alcohol and Depression Cycle
For people living with clinical depression, especially if it’s undiagnosed or untreated, drinking can feel like an escape. Using alcohol to numb sadness or loneliness may provide short-term relief, but it often creates a vicious cycle of negative emotions and dependency. In fact, more than 30% of people with alcohol use disorder experience this cycle firsthand.
Can Alcohol Cause Depression? Or Does Depression Cause Drinking?
The answer to both questions is “yes.” Research shows that people with depressive disorders often turn to alcohol as a way to cope with their symptoms. However, long-term alcohol use can lead to dependency and worsen depressive symptoms. Similarly, drinking can exacerbate depression symptoms because alcohol is a depressant that slows brain functioning and disrupts the balance of neurotransmitters responsible for managing emotions.
In fact, the connection between drinking and depression has become so significant that the DSM-5 now includes a new subsection of depressive disorders called “Substance/Medication-Induced Depressive Disorder.” This disorder is characterized by a prominent and persistent disturbance in mood caused by the use of substances and/or medications.
Breaking The Cycle
Breaking the cycle of alcohol use and depression requires commitment and support. Here are some tips to help you get started:
- Know your resources. Treatment centers offer various options, including therapy sessions, family therapy, and pharmacological treatments. These comprehensive programs focus on clinical depression and substance abuse. Cognitive Behavioral Therapy (CBT) is designed to help you become aware of feelings that cause depression and a desire to use alcohol. It also helps teach coping skills that you can use to live a healthier lifestyle. Medication-assisted therapy may combine talk-therapy tactics with prescribed medications like naltrexone that help alleviate withdrawal and reduce the risk of relapse.
- Join a support group. Peer-support groups have been shown to have a positive impact on the treatment of alcoholism and depression. They offer access to new perspectives and skills you may not have thought of before, and can remind you that you are not alone in your journey to recovery.
- Consider inpatient/outpatient recovery programs. These programs are available for both alcohol addiction and depression. They allow you to connect with others with similar experiences and provide professional support to help you throughout your recovery.
- Make changes in your lifestyle. Smaller-scale changes, combined with emotional support from family and friends, can make all the difference in improving your mental health. Exercise regularly to boost your mood, get a healthy amount of sleep to improve your overall well-being, develop stress-reducing and relaxation skills, and surround yourself with people who care and support your recovery.
At Eleanor Health, we offer care and treatment that takes into account the whole individual, meaning that we focus on one’s life experiences, cultures, and values when offering assistance. With resources available in medication-assisted treatment, therapy & counseling, psychiatry, recovery coaching, and more, we are dedicated to helping you get to a place where you feel happy and healthy.
If you are seeking help with your loved one’s addiction, contact us today or complete our quick contact form below to speak with an addiction treatment specialist.
If you need help with your substance use disorder, we are here to help you build your confidence and momentum towards the future you want. We provide online treatment services for adults with alcohol, opioid, and other substance use disorders.